Suman Majumdar, Philipp du Cros
Burnet Institute and Department of Infectious Diseases, Alfred Hospital, Melbourne VIC
Last reviewed: October 2019
Introduction
Tuberculosis (TB) is an airborne infectious disease caused by Mycobacterium tuberculosis and is an acquired immune deficiency syndrome (AIDS)-defining illness in Australia and other high-income countries. TB remains a global health crisis with an estimated 10 million new cases and 1.6 million deaths occurring each year. The intersection of the TB and human immunodeficiency virus (HIV) epidemics has contributed to an increase in the global TB burden, with 9% of all new TB cases occurring in people with HIV infection in 2017.1 Globally, TB is the most common presenting illness and leading cause of mortality in people with HIV infection, accounting for 1 in 3 of deaths.The emergence and transmission of multidrug-resistant (MDR, resistance to at least isoniazid and rifampicin) M. tuberculosis is a growing challenge, particularly for the Asia-Pacific region.
Australia has one of the lowest TB case notification rates in the world (5.7 cases per 100,000 population in 2014) with higher rates in indigenous Australians (6 times the rate of the non-indigenous population). Eighty-six per cent of TB cases occur in overseas-born persons, making this the most significant risk factor.4 Accordingly, HIV-associated TB in Australia is mainly found in overseas-born people. In 2014, HIV testing occurred in 82% of reported TB cases, among them 55% had a result reported and among them, 2% were (17 cases) were identified as being HIV positive.4
Tuberculosis infection ensues when airborne droplets containing M. tuberculosis from an infectious host are inhaled, taken up by alveolar macrophages at the terminal airways and encounter the immune system. The conventional model considered TB to be a binary state between latent TB infection (LTBI), an inactive, non-infectious state, and active disease, the infectious form where clinical signs and symptoms are present. Transitions between the binary states result in one of three clinical outcomes – primary disease, TB infection and reactivation or post-primary disease. There is no gold standard test for direct identification of M. tuberculosis infection in humans. (LTBI is defined as the absence of active TB disease and evidence of an antigen-specific T cell response to mycobacterial proteins measured by reactivity in the tuberculin skin test (TST, also known as a Mantoux test) or an interferon-gamma release assay (IGRA). Active disease is classified as either primary TB (involving progression 1-2 years following infection due to loss of immune containment) or reactivation TB (also known as post primary) with disease following infection resulting from LTBI previously seeded at the time of primary infection. Approximately one-quarter of the world’s population is estimated to have M. tuberculosis infection and 90-95% of these people (HIV negative, no other risk factors) will not develop active disease, indicating that the human immune system can control M. tuberculosis infection. It is estimated that 5.1% of the Australian population had LTBI in 2016.
A conceptual scientific shift has occurred to view M. tuberculosis infection as a continuous spectrum spanning eliminated infection (early clearance by innate immune responses or delayed clearance by adaptive immune responses), LTBI (quiescent infection with immune containment), subclinical active disease and fulminant active disease (see figure 1). However, significant biomedical knowledge gaps exist in the understanding of the factors that govern infection, pathogenesis and progression to active disease (the host-pathogen interaction). This has resulted in a lack of adequate biomarkers to measure states of infection and disease and therapeutic targets for preventive, diagnostic and therapeutic tools for TB and TB-HIV co-infection. Many prefer to use the term TB infection, rather than LTBI as latent may imply that management or treatment is not needed. Further, not all who are considered to clinically have LTBI (e.g. household contracts) and receive treatment, are tested or have a positive result. However, for simplicity in clinical and public health settings, patients are usually categorized as having either LTBI or active TB disease.
Figure 1. The spectrum of TB, from Mycobacterium tuberculosis infection to active (pulmonary) TB disease.
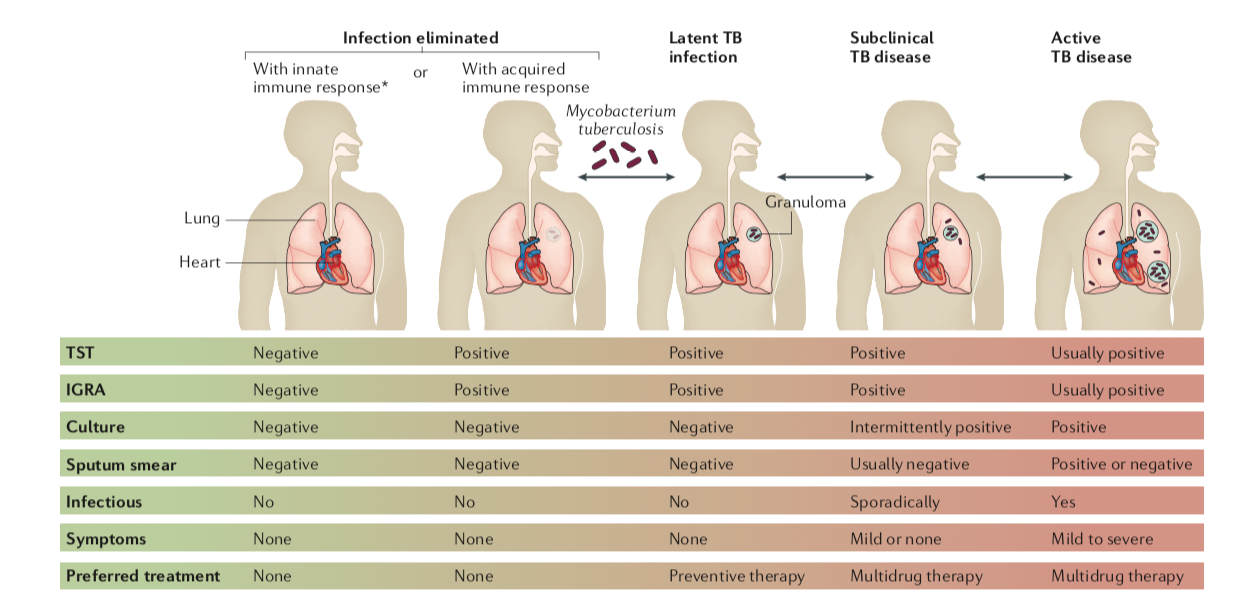
Source: Pai M, Behr M, Dowdy D, et al. Tuberculosis. Nat Rev Dis Primers
2016; 2: 16076. Used with permission.

